[ad_1]

Get vaccinated from shingles – a painful debilitating condition that can burn out years after infection from the water cell zone – may not only reduce the risk of infection, but also provide some protection against dementia, suggesting new provocative studies.
A new study published in nature on Wednesday, analysing data from more than 280,000 seniors in Wales, finding that those who received the original shingles vaccine are 20% less likely to develop a type of dementia than those who have not been vaccinated.
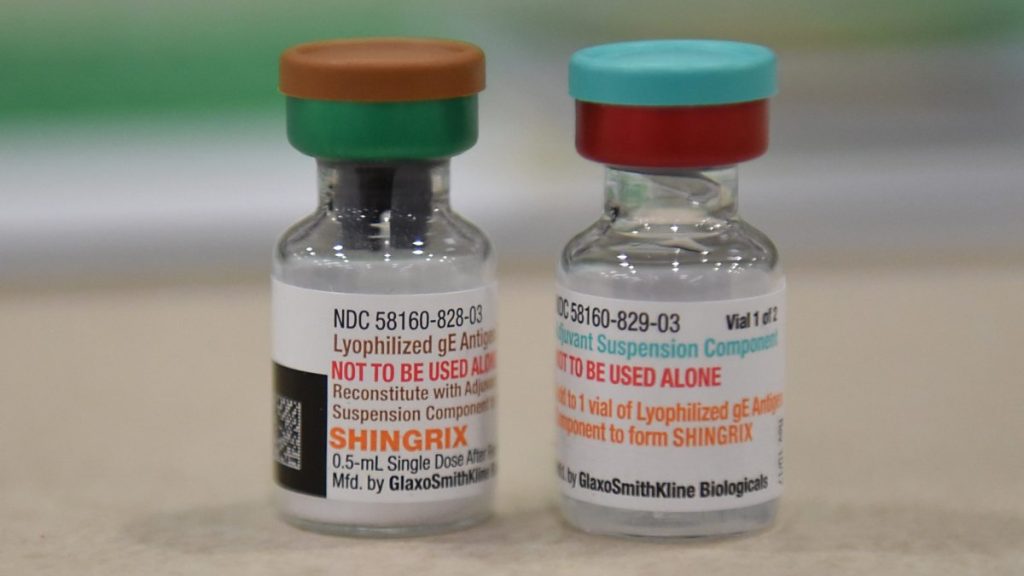
Previous studies have found an association between Singlix’s iron-bladed vaccine, which replaces the 2020 live virus version, and a lower risk of dementia, particularly among women. However, the study design was not considered strong because the vaccinated people could not explain the potential differences between those who were vaccinated and those who were not. ShingRex, which targets a small number of viral DNA, has been found to last longer than the original vaccine.
Wales’ unusual public health policies allowed new research that provided “natural experiments” to investigate the potential impact of vaccines on the risk of dementia. The deployment of the vaccine in Wales in 2013 provided shots to those born after September 2, 1933, but none were born by that date.
This allowed researchers at Germany and Stanford University to compare two groups of people with similar health characteristics that differ only for one week, making the vaccine essentially the same except that they are available to younger populations but not older people, said Dr. Pascal Geldsetzer, an assistant professor of medicine at Stanford University and a senior author of the study.
What’s exciting about this study is that it’s like a randomized controlled trial that is considered the gold standard for research.
Alison Aiello, an epidemiology professor at Columbia University Aging Center in New York City, said the way the original vaccine was deployed in Wales provided a unique opportunity.
“It’s like having a control group compared to the treated group,” said Aiero, who has nothing to do with the new study. “What’s interesting is the discovery of 20% protection. It’s a very powerful effect and fits into other studies that suggest that the herpes virus can affect dementia.”
Scientists don’t know exactly how the chicken po virus increases the risk of dementia. For example, it has been shown that virus reactivation can lead to the accumulation of abnormal proteins associated with Alzheimer’s disease, Geldsetzer said. The virus can also cause the reactivation of herpes simplex. This is what previous research is related to dementia.
Herpes virus does not disappear completely, but it lurks inside the body until the immune system weakens. Aging leads to a natural weakening of the immune system, allowing the virus to resurface as shingles as shingles.
The age effect is given as two doses of 2 to 6 months, the reason why the shingles vaccine is only available to people over 50 in the United States.
Herpes viruses, including herpes simplex, appear to have the ability to enter the central nervous system, experts said.
In fact, a 2024 study found that among 70-year-olds who initially had no dementia, older adults diagnosed with herpes simplex are more than twice as many infections as they develop dementia over a 15-year follow-up.
Herpes simplex can cause havoc if you pass through a barrier to the blood-brain. It can cause inflammation of both meninges (meningitis) and brain (encephalitis). Both are fatal.
The intensifying cases of the shingles vaccine protecting against dementia came from a study published in Nature Medicine in 2024, which analyzed medical records from over 100,000 patients. The analysis suggests that the new shingles vaccine is associated with even better protection against dementia.
In that study, the researchers also investigated whether two other vaccines, influenza and tetanus, diphtheria and pertussis, had an impact on the risk of dementia. They didn’t.
The most important takeaway message from Stanford University research is that getting vaccinated can reduce the risk of dementia, said Dr. Arrati Didowania, professor of medicine and medical education at Feinberg School of Medicine at Northwestern University in Chicago.
It is not clear how the vaccine will protect against dementia, Didwania said. “But that’s an interesting question,” she added. “Is it by reducing inflammation or preventing the virus from reactivating?”
There is certainly a good reason to get vaccinated, Didwania said.
“Shimpers zoster is a severe, painful, debilitating condition that can lead to horrible, long-term pain,” she said.
New research has limitations. Dr. William Schaffner, a professor of infectious diseases at Vanderbilt University Medical Center in Nashville, Tennessee, said that while it shows the benefits of vaccines in real-world settings, it is not the same as randomized controlled trials. But it would not be ethical to randomly assign people to get the vaccine.
“It’s provocative, interesting and exciting,” he said of the research.
The Food and Drug Administration has reviewed studies linking the shiny vaccine to a lower risk of dementia, allowing pharmaceutical companies to add signs to their labels, Schaffner said.
Even if that doesn’t happen, doctors can use the findings to convince patients to choose to vaccinate.
“Obviously there are a lot of people over 50 who haven’t received the vaccine,” he said. “If people say there’s data that suggests that vaccines will prevent some cases of dementia, people might be persuaded.”
This story first appeared on nbcnews.com. More from NBC News:
[ad_2]Source link